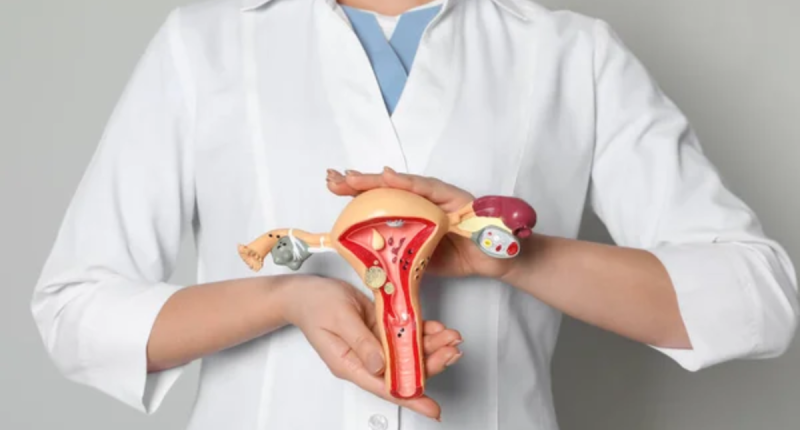
PID, or pelvic inflammatory disease (PID) is one of the most common serious infections of the female reproductive tract in the United States, Centers for Disease Control and Prevention (CDC). It can damage the uterus, fallopian tubes, and ovaries, and can lead to infertility if left untreated. It is estimated that 1 in 8 women will develop PID at some point in their lifetime.
PID is most often caused by sexually transmitted infections (STIs) such as chlamydia and gonorrhea, but it can also be caused by other types of bacteria.
Statistical facts
- PID is most common in women aged 15 to 25 years.
- In 2018, an estimated 770,000 women in the United States had PID.
- Black women are more likely to develop PID than women of other races or ethnicities.
- Women who live in poverty are also more likely to develop PID.
PID can have serious consequences, including infertility, chronic pelvic pain, and ectopic pregnancy. However, early diagnosis and treatment can help to prevent these complications.
Here are some additional statistics about PID:
- About 10% to 15% of women with untreated chlamydia or gonorrhea will develop PID.
- About 80% of women with PID have had a previous STI.
- About 20% to 30% of women with PID will experience infertility.
- About 10% of women with PID will have a chronic pelvic pain.
- About 2% of women with PID will have an ectopic pregnancy.
Symptoms of Pelvic Inflammatory Disease
The symptoms of PID can vary from mild to severe. Some women may not experience any symptoms at all. However, the most common symptoms include:
- Lower abdominal pain or pelvic pain
- Painful sex
- Unusual vaginal discharge, often with a foul odor
- Fever
- Painful urination
- Bleeding between periods
Causes of PID
PID is usually caused by bacteria that travel from the vagina to the uterus, fallopian tubes, and ovaries. The most common bacteria that cause PID are:
- Neisseria gonorrhoeae (gonorrhea)
- Chlamydia trachomatis (chlamydia)
- Mycoplasma genitalium
- Gardnerella vaginalis
- Bacteroides species
Other bacteria that can cause PID include those that normally live in the vagina and cervix. These bacteria can cause PID if they enter the upper reproductive tract during or after childbirth, miscarriage, abortion, or gynecological surgery.
Risk factors for PID
Women who are at increased risk for PID include:
- Women under the age of 25
- Women who have multiple sexual partners
- Women who do not use condoms during sex
- Women who have a history of STIs
- Women who have recently had an intrauterine device (IUD) inserted or removed
- Women who have recently had a miscarriage, abortion, or gynecological surgery
Diagnosis of PID
Pelvic inflammatory disease (PID) can be difficult to diagnose because the symptoms are similar to those of other conditions, such as appendicitis, kidney infections, and ovarian cysts. To diagnose PID, a healthcare provider will typically perform a pelvic exam and order laboratory tests.
Pelvic exam – During a pelvic exam, the healthcare provider will insert two gloved fingers into the vagina to check for tenderness, swelling, and abnormal discharge. They may also use a speculum to widen the vagina and view the cervix.
Laboratory tests – The following laboratory tests may be ordered to help diagnose PID:
- Blood test: A blood test can check for white blood cell count, which is elevated in infection.
- Urine test: A urine test can check for white blood cells, bacteria, and other signs of infection.
- Vaginal culture: A vaginal culture can identify the bacteria that is causing the infection.
In some cases, additional tests may be ordered, such as:
- Ultrasound: An ultrasound can be used to visualize the uterus, fallopian tubes, and ovaries and check for signs of infection, such as abscesses.
- Laparoscopy: Laparoscopy is a minimally invasive surgical procedure that allows the healthcare provider to view the pelvic organs directly. This may be necessary to confirm the diagnosis of PID or to rule out other conditions.
Criteria for diagnosis
The diagnosis of PID is based on the following criteria:
- Clinical evidence of lower genital tract inflammation, such as mucopurulent cervical discharge, cervical friability, or cervical motion tenderness
- Evidence of upper genital tract inflammation, such as adnexal tenderness, adnexal masses, or elevated temperature
At least one of the following:
- A positive test for chlamydia or gonorrhea
- Elevated white blood cell count or C-reactive protein level
- Evidence of endometritis on endometrial biopsy
- Abscess formation on ultrasound or laparoscopy
Treatment options for PID
The treatment for pelvic inflammatory disease (PID) depends on the severity of the infection and the type of bacteria that caused it. In most cases, PID can be treated with antibiotics on an outpatient basis. However, in some cases, hospitalization may be necessary.
Antibiotics – The type of antibiotic and the duration of treatment will depend on the type of bacteria that caused the infection. Commonly used antibiotics for PID include:
- Ceftriaxone (Rocephin)
- Doxycycline (Vibramycin)
- Levofloxacin (Levaquin)
- Metronidazole (Flagyl)
- Ofloxacin (Floxin)
Most women with PID will need to take antibiotics for at least two weeks. It is important to take all of the medication prescribed by your doctor, even if you start to feel better sooner.
Other treatments – In addition to antibiotics, your doctor may also recommend other treatments for PID, such as:
- Pain medication: Over-the-counter pain relievers such as ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) can help to relieve pain and inflammation.
- Rest: Getting plenty of rest can help your body to fight off the infection.
- Fluids: Drinking plenty of fluids will help to prevent dehydration.
Hospitalization
Hospitalization may be necessary for women with severe PID, such as those with:
- Fever over 101 degrees Fahrenheit
- Severe abdominal pain
- Signs of abscess formation
- Inability to take antibiotics by mouth
In the hospital, you will receive antibiotics through an IV (intravenous) line. You may also need surgery to drain an abscess.
Follow-up care
It is important to follow up with your doctor after treatment for PID to make sure that the infection is gone and that you are not experiencing any complications.
Complications of PID
PID can lead to serious complications, such as:
- Infertility
- Chronic pelvic pain
- Ectopic pregnancy
- Tubo-ovarian abscess (a collection of pus in the fallopian tubes and ovaries)
- Sepsis (a life-threatening infection of the bloodstream)
If you experience any of the following symptoms after treatment for PID, it is important to see your doctor right away:
- Fever
- Abdominal pain
- Vaginal discharge
- Painful urination
- Bleeding between periods
Early diagnosis and treatment of PID can help to prevent serious complications.
Prevention
The best way to prevent PID is to practice safe sex and get regular checkups.
Safe sex
- Use condoms during all sexual activity, regardless of whether you are having vaginal, anal, or oral sex.
- Get tested for STIs regularly, especially if you have new sexual partners.
- Avoid having sex with multiple partners at the same time.
Other prevention options
- Avoid douching, which can upset the natural balance of bacteria in the vagina.
- Wipe from front to back after using the toilet to prevent bacteria from the anus from entering the vagina.
- Get vaccinated against human papillomavirus (HPV).
Regular checkups
See your doctor for regular checkups and Pap tests. This will help to catch any STIs or other problems early on, when they are most treatable.
If you have any of the following risk factors for PID, it is especially important to take steps to prevent it:
- Under the age of 25
- Multiple sexual partners
- No condom use
- History of STIs
- Recently had an intrauterine device (IUD) inserted or removed
- Recently had a miscarriage, abortion, or gynecological surgery
If you think you may have PID, it is important to see a doctor right away. Early diagnosis and treatment can help to prevent serious complications.
Here are some additional tips to help prevent PID:
- Talk to your doctor about your sexual history and risk factors for PID.
- Ask your doctor about the best way to prevent PID based on your individual needs.
- Be honest with your sexual partners about your sexual history and risk factors for PID.
- Encourage your sexual partners to get tested for STIs.
By taking these steps, you can help protect yourself from PID and other serious health problems.
Don’t miss: Human Papillomavirus (HPV) Everything You Should Know