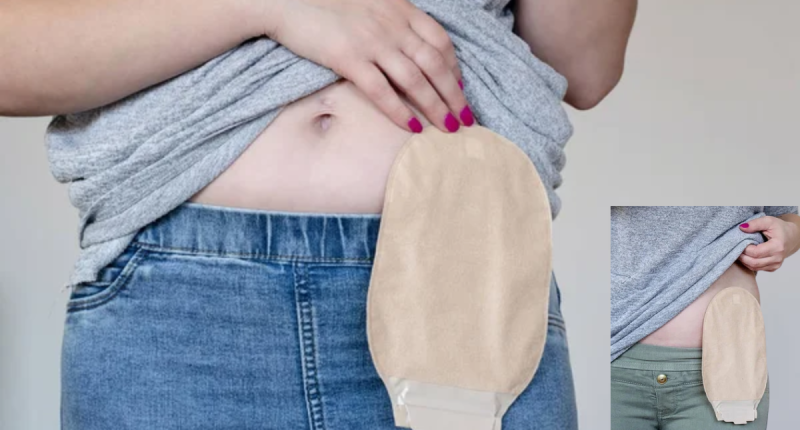
What Happens To Your Anus After Colostomy? After a colostomy, the anus may still function normally, or it may not. This depends on the type of colostomy that was performed and the reason for the surgery.
In a temporary colostomy, the anus is typically left intact and will continue to function normally. This means that you will still be able to pass stool and gas through your anus. However, you may also have some discharge from your anus, which is usually mucus or dead cells from the lining of the bowel.
In a permanent colostomy, the anus may be closed off or removed. This means that you will no longer be able to pass stool or gas through your anus. You will instead have to wear a colostomy bag to collect stool and gas that exits through the stoma.
Here is a table summarizing the possible effects of a colostomy on the anus:
| Type of colostomy | Anus function | Possible discharge |
|---|---|---|
| Temporary | Normal | May have some mucus or dead cells from the lining of the bowel |
| Permanent | Closed off or removed | No stool or gas |
Here are some specific changes that may occur to the anus after a colostomy:
- Mucus production: The anus may continue to produce mucus, even though it is no longer serving its original purpose. This mucus may leak out of the anus or you may feel the urge to go to the toilet. The mucus is normally clear or white and looks like egg white or glue.
- Sensation: The anus may still have some sensation, even after a colostomy. This means that you may still be able to feel the urge to have a bowel movement, even though you will no longer be able to control it.
- Control of gas: In some cases, you may still be able to control gas to some extent after a colostomy. However, you may not have complete control, and you may experience some leakage of gas.
Colostomies can be performed in different parts of the colon:
- Ascending colostomy: This type of colostomy is done on the right side of the abdomen, near the hipbone.
- Transverse colostomy: This type of colostomy is done on the upper abdomen, across the waist.
- Descending colostomy: This type of colostomy is done on the left side of the abdomen, near the lower ribs.
- Sigmoid colostomy: This type of colostomy is done on the lower left abdomen, near the pelvic bone.
The type of colostomy that is right for you will depend on the specific reason for your surgery and the location of the problem in your colon.
After a colostomy, you will need to learn how to care for your stoma and wear a colostomy bag. You will also need to make some changes to your diet and lifestyle. However, with proper care and support, you can live a full and active life with a colostomy.
Colostomy complications
Stoma complications:
These complications can affect the stoma itself and the surrounding skin. They include:
- Stoma prolapse: This occurs when the stoma protrudes through the opening in the abdomen.
- Stoma retraction: This occurs when the stoma sinks back into the abdomen.
- Stoma stricture: This occurs when the stoma narrows, making it difficult for stool to pass through.
- Stoma ischemia: This occurs when the stoma does not receive enough blood flow, which can lead to tissue death.
- Parastomal hernia: This occurs when a portion of the intestine protrudes through a weakened area in the abdominal wall near the stoma.
Skin complications
These complications can affect the skin around the stoma. They include:
- Skin irritation: This is caused by the adhesive used to attach the colostomy bag to the skin.
- Skin infection: This can be caused by bacteria that enter the skin through a cut or sore.
- Fungal infection: This can be caused by fungus that grows in the warm, moist environment around the stoma.
Other complications:
These complications can affect other parts of the body. They include:
- Dehydration: This can occur if you lose too much fluid through the stoma.
- Electrolyte imbalance: This can occur if you lose too many electrolytes, such as sodium, potassium, or chloride, through the stoma.
- Intestinal obstruction: This can occur if the intestine becomes blocked, preventing stool from passing through.
- Stoma fistula: This is a hole that develops between the stoma and another part of the intestine.
Preventing complications
There are a number of things you can do to help prevent complications from a colostomy. These include:
- Following your doctor’s instructions carefully: This includes taking your medications as prescribed and caring for your stoma properly.
- Eating a healthy diet: This will help to keep your stools formed and easy to pass.
- Getting regular exercise: This will help to keep your bowels regular and prevent constipation.
- Avoid lifting heavy objects: This can put a strain on the abdominal wall and increase the risk of a hernia.
- Seeing your doctor for regular checkups: This will help to identify and treat any complications early on.
Additional tips that may help to prevent specific complications:
To prevent skin irritation:
- Use a barrier cream or wipe around the stoma to protect the skin.
- Change your colostomy bag as often as recommended by your doctor.
- Gently pat the skin around the stoma dry after showering or bathing.
To prevent stoma blockage:
- Eat a high-fiber diet.
- Drink plenty of fluids.
- Avoid foods that are high in insoluble fiber, such as nuts, seeds, and popcorn.
- If you experience constipation, talk to your doctor about stool softeners or laxatives.
To prevent parastomal hernia:
- Avoid lifting heavy objects.
- Maintain a healthy weight.
- Wear a support garment, such as a hernia belt, if recommended by your doctor.
Colostomy symptoms
Here are some of the common symptoms of a colostomy:
- Stoma blockage:
- Not passing stool or gas
- Bloating and swelling in the abdomen
- Abdominal cramps
- Nausea and vomiting
- Skin irritation:
- Redness, swelling, and pain around the stoma
- Itching or burning around the stoma
- A rash around the stoma
- Wound infection:
- Redness, swelling, and pain around the incision
- Pus or drainage from the incision
- Fever
- Stoma prolapse:
- A bulge in the abdomen around the stoma
- Pain or discomfort when lifting or straining
- Parastomal hernia:
- A bulge in the abdomen around the stoma
- Pain or discomfort when lifting or straining
- Fistula:
- Leakage of stool or gas from the fistula
- Pain or discomfort in the abdomen
Colostomy causes
There are many different causes of a colostomy, including:
- Bowel cancer: This is the most common reason for a colostomy. When bowel cancer is diagnosed early, it can often be treated successfully with surgery. However, if the cancer has spread to other parts of the body, a colostomy may be necessary to relieve the symptoms of the cancer and improve quality of life.
- Inflammatory bowel disease (IBD): IBD is a group of chronic conditions that cause inflammation of the digestive tract. The two most common types of IBD are Crohn’s disease and ulcerative colitis. A colostomy may be necessary if IBD causes severe inflammation or blockage of the colon.
- Diverticulitis: Diverticulitis is an inflammation of small pouches (diverticula) that form in the walls of the colon. Diverticulitis can cause severe pain, bleeding, and infection. A colostomy may be necessary if diverticulitis causes a perforation or abscess in the colon.
- Colorectal polyps: Colorectal polyps are growths that form on the inner lining of the colon. Most colorectal polyps are harmless, but some can develop into cancer. A colostomy may be necessary if a polyp is large or has a high risk of developing into cancer.
- Rectal prolapse: Rectal prolapse is a condition in which the rectum protrudes through the anus. This can be caused by weakened muscles and ligaments in the pelvic floor. A colostomy may be necessary if rectal prolapse is severe and cannot be treated with other methods.
Less common reasons for a colostomy.
- Injuries to the colon or rectum: Injuries to the colon or rectum can be caused by accidents, trauma, or surgery. A colostomy may be necessary if an injury has caused a perforation or blockage of the colon.
- Birth defects: Some birth defects can affect the development of the colon or rectum. A colostomy may be necessary if a birth defect prevents stool from passing normally.
- Other medical conditions: Other medical conditions, such as Hirschsprung’s disease and fecal incontinence, may also require a colostomy.
Continue to check our website soundhealthandlastingwealth.com for the next article loop colostomy and, please use our comment section as well, we would love to hear from you.
Resources:
1. Coping with a colostomy after anal cancer: Cancer Research UK
2. Colostomy: Mayoclinic
3. Colostomy overview: Sciencedirect