The 4 Best Workouts for Men To Build Muscle Mass in 30 Days – Building a solid, classic male physique first and foremost requires muscle mass. Regardless of whether you want to look like Brad Pitt from “Fight Club” or Dwayne Johnson from any movie he’s been in, increasing your muscle mass is priority number one. While there’s a ton of misinformation and general “noise” when it comes to how to build muscle mass, the truth is that sculpting muscle is not particularly complicated. We’re here to help and rounded up the best workouts for men to build muscle mass in 30 days. (You can thank us later!)
To put it simply, you need to work out with moderate to heavy weights using exercises that target the various muscle groups in your body. Generally speaking, you want to hit the major muscle groups in your chest, shoulders, back, and legs. Your core muscles and arm muscles also deserve some attention, but the primary focus should be on the bigger muscles involved in compound movements.
In this article, we bring you the most productive workouts for men to build muscle mass in 30 days. This routine is designed with four workouts per week. Perform each workout once per week. You can perform back-to-back workouts, but always allow at least one rest day between back-to-back workout days. For example, you could perform workouts #1 and #2 on Monday/Tuesday, and workouts #3 and #4 on Thursday/Friday. Ultimately, you will need to perform at least two days back-to-back in order to hit the weekly workouts, but remember—muscle growth and recovery happen during rest, not during the workout itself.
Be sure to eat a healthy, high-protein diet and get enough water and sleep to ensure you actually get the gains. Keep reading for our best workouts for men to build muscle mass in 30 days. And next, be sure to read Is Orange Juice Good For You? Here’s What the Science Says
Workout #1: Legs, Shoulders, Triceps

The following workout combines lower-body leg exercises with upper-body shoulder exercises and finishes with triceps.
Barbell Squats
For this first exercise, stand with a barbell racked across your upper back, your feet shoulder-width apart, and your toes pointing slightly outward. Keep your chest up and your core engaged as you push your hips back and bend your knees. Lower your body until your thighs are parallel to the ground or slightly below. Push through your feet to return to the starting position, fully extending your hips and knees. Repeat for the target repetitions.
Dumbbell Overhead Press

Next, stand with your feet shoulder-width apart, holding dumbbells at shoulder height with your palms facing forward. Engage your core and your glutes to stabilize your lower back, and push the weight overhead, fully extending your arms. Lower the weight back to the starting position in a controlled manner. Repeat for the target repetitions.
Dumbbell Lunges
For dumbbell lunges, you’ll stand with your feet hip-width apart and your hands on your hips or holding dumbbells at your sides. Take a step forward with your right foot. Bend both knees to lower your body until your right thigh is parallel to the ground and your left knee is hovering above the floor. Rotate your left foot inward slightly as you lower your left knee for optimal biomechanics. Push through your right foot and step back to the starting position. Repeat for the target repetitions, then switch legs.
Dumbbell Lateral Raise
The dumbbell lateral raise will have you starting with a dumbbell in each hand, held at your sides, palms facing inward. Raise the dumbbells to the sides until your arms are parallel to the ground, keeping a slight bend in your elbow. Slowly return to the starting position. Repeat for the target repetitions.
Triceps Rope Pushdown
For the final exercise in this first workout, attach a rope to a high pulley on a cable machine and grasp the ends of the rope with both hands, palms facing each other. Stand facing the machine with your elbows tucked close to your body and bent at a 90-degree angle. Engage your core, and maintain a slight bend in your knees for stability. Push the rope down, extending your elbows until your arms are fully straightened. Squeeze your triceps at the end range for about one second. Slowly return to the starting position. Repeat for the target repetitions.
Workout #2: Chest, Back

Next up in our workouts for men to build muscle features exercises that work the chest and back.
Dumbbell Bench Press
To perform a dumbbell bench press, lie on a flat bench with a dumbbell in each hand, palms facing away from your body. Position the dumbbells at chest level with your elbows bent at a 90-degree angle. Press the dumbbells up and together, fully extending your arms and contracting your chest muscles. Slowly lower the dumbbells back down to the starting position, controlling the movement. Repeat for the target repetitions.
Dumbbell Row

To set up for the dumbbell row, stand with your feet hip-width distance apart and hold a dumbbell in one hand, palm facing inward. Bend forward at the hips, keeping your back straight and your knees slightly bent. Place your free hand on a bench or your thigh for support, and let the dumbbell hang directly below your shoulder. Pull the dumbbell up toward your ribcage, retract your shoulder blade, and visualize crushing a piece of fruit in your armpit at the end range of motion. Lower the dumbbell back to the starting position in a controlled manner. Repeat for the target repetitions
Dumbbell Incline Press
To perform a dumbbell incline press, sit on an incline bench set at a 30- to 45-degree angle with a dumbbell in each hand, thumbs facing each other. Position the dumbbells at chest level with your elbows bent at a 90-degree angle. Press the dumbbells up and together, fully extending your arms and contracting your chest muscles. Slowly lower the dumbbells back down to the starting position, controlling the movement and avoiding shrugging throughout the range of motion. Repeat for the target repetitions.
Seated Cable Row
To perform a seated cable row, sit on the cable row machine with your feet on the footplate and your knees slightly bent. Grasp the handle with both hands, palms facing each other. Engage your core and sit up straight, keeping your back neutral. Pull the handle toward your abdomen, retract your shoulder blades, and visualize crushing a piece of fruit in your armpit at the end range of motion. Slowly return to the starting position, maintaining tension on your back muscles throughout the movement. Repeat for the target repetitions.
Workout #3: Legs

Barbell Deadlift
To perform a barbell deadlift, stand with your feet shoulder-width distance apart, with the barbell positioned over the middle of your feet. Bend at the hips and knees to grip the barbell, with your hands just outside your knees. Engage your lats, pull your shoulder blades down and back, and brace your core. Push your feet into the floor, extending your hips and your knees simultaneously to lift the barbell off the ground. Keep the bar close to your body throughout the movement. Once fully standing, reverse the movement to lower the barbell back to the ground. Repeat for the target repetitions.
Barbell Hip Thrust
Begin this next exercise by sitting on the ground with your back against a bench, feet flat on the floor, and a barbell positioned across your hips. Visualize drawing your lower rib toward your pelvis, engaging your abs. Push through your feet, and lift your hips off the ground, extending them fully while keeping your upper back on the bench. Squeeze your glutes at the top of the movement for about one second. Lower your hips back to the starting position in a controlled manner. Repeat for the target repetitions.
Leg Press

To perform a leg press, sit on the leg press machine with your back and head resting against the padded support. Place your feet on the platform hip-width distance apart with your knees bent at a 90-degree angle. Engage your core, and push through your feet into the platform to extend your legs, keeping your feet flat on the platform. Slowly return to the starting position, allowing the weight to come down without touching the weight stack. Repeat for the target repetitions.
Quad Extension
To perform a quad extension, sit on a leg extension machine with your back against the pad, and adjust the roller pad to rest just above your ankles. Grasp the handles on the sides of the machine for stability, and engage your core. Extend your legs fully, squeezing your quadriceps at the end range for about one second. Slowly lower the weight back to the starting position, keeping tension on your quadriceps throughout the movement. Repeat for the target repetitions.
Hamstring Curl
To perform a hamstring curl, lie face down on a leg curl machine with your legs fully extended and the roller pad positioned just above your ankles. Grasp the handles on the sides of the machine for stability, and engage your core. Curl your legs up toward your glutes, squeezing your hamstrings at the end range for about one second. Slowly return to the starting position, maintaining tension on your hamstrings throughout the movement. Repeat for the target repetitions.
Workout #4: Back, Biceps, Core

The last of our workouts for men to build muscle mass in 30 days targets the back, biceps, and core.
Wide Grip Pull-up
To perform a wide grip pull-up, grasp a pull-up bar with a wide, prone grip, palms facing away from you. Hang from the bar with your arms fully extended and your legs slightly bent. Engage your core, and visualize crushing a piece of fruit in your armpit and pulling your elbows toward the floor as you pull your body up to the bar. Continue pulling until your chest hits the bar, then slowly lower yourself back down to the starting position. Repeat for the target repetitions.
Parallel Pull-up
Grasp a pull-up bar with a parallel grip, palms facing each other and your hands shoulder-width apart. Hang onto the bar with your arms fully extended and your legs slightly bent. Engage your core, and visualize crushing a piece of fruit in your armpit as you pull your body up toward the bar. Continue pulling until your chest hits the bar, then slowly lower yourself back down to the starting position. Repeat for the target repetitions.
Lat Pulldown
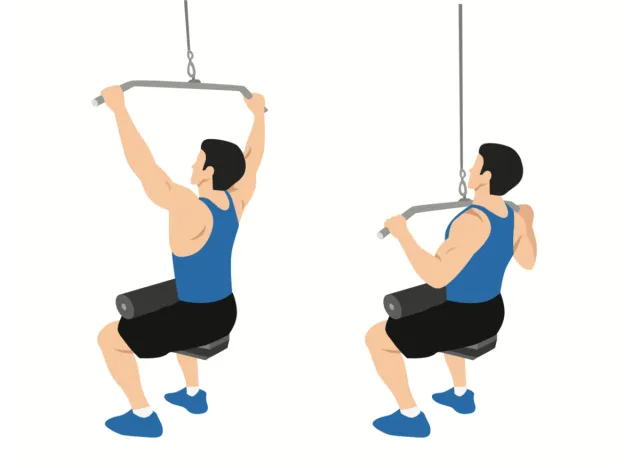
To perform a lat pulldown, sit on a lat pulldown machine with your thighs secured under the pads, and grasp the bar with a wide grip, palms facing away from you. Lean back slightly, and engage your core, keeping your spine neutral. Pull the bar down toward your upper chest, retract your shoulder blades, and picture crushing a piece of fruit in your armpit at the end range of motion. Slowly return the bar to the starting position, maintaining tension on your back muscles throughout the movement. Repeat for the target repetitions.
Bicep Curl
To perform a bicep curl, stand with your feet hip-width distance apart, holding a dumbbell in each hand with your palms facing forward. Keep your elbows close to your body, and maintain a slight bend in your knees for stability. Curl the dumbbells up toward your shoulders, squeezing your biceps at the top of the movement for about one second. Slowly return to the starting position. Repeat for the target repetitions.
Hammer Bicep Curl
To perform a hammer bicep curl, stand with your feet hip-width distance apart, holding a dumbbell in each hand with your palms facing inward. Keep your elbows close to your body, and maintain a slight bend in your knees for stability. Curl the dumbbells up toward your shoulders while keeping your palms facing inward throughout the movement. Squeeze your biceps at the top of the movement for about one second, then slowly lower the dumbbells back to the starting position. Repeat for the target repetitions.
Hanging Leg Raise
To perform a hanging leg raise, hang onto a pull-up bar with your hands shoulder-width apart and your legs fully extended. Engage your core, and maintain a slight bend in your knees for stability. Lift your legs up toward your chest, keeping your legs as straight as possible and your feet flexed. Slowly lower your legs back to the starting position in a controlled manner. Repeat for the target repetitions.
Russian Twist
To round out our best workouts for men to build muscle mass in 30 days, it’s time to wrap up with the Russian twist. Sit on the ground with your knees bent and your feet flat on the floor, and hold a dumbbell, medicine ball, or weight plate with both hands. Lean back slightly, engage your core, and lift your feet off the ground. Do not cross your ankles. Twist your torso to one side, tapping the weight on the ground next to your hip. Rotate your torso to the opposite side, tapping the weight on the ground next to your other hip. Repeat for target repetitions.









