
The #1 Daily Walking Workout for Women to Get Fit – If you’re not walking regularly, you’re missing out on one of the most underappreciated tools for a toned and fit body. While high-intensity workouts and endurance activities often steal the spotlight, walking humbly stands its ground, continuing to prove its weight loss benefits time and time again. A 2022 study published in Nutrients found that postmenopausal women with a regular walking routine experienced weight loss regardless of walking speed. So, for women who are looking to sculpt their fittest bodies, incorporating a daily walking routine can be a total game-changer. We have the ultimate daily walking workout for women to get fit.
Walking offers a unique blend of benefits. It’s gentle on the joints, can be done anywhere, and requires no fancy equipment. But here’s the twist: Not all walking workouts are created equal. That’s why we chatted with Tracie Haines-Landram, CSCS, a certified strength and conditioning specialist and nutrition coach with Barbend, who reveals the #1 daily walking workout for women to achieve their fitness goals. The best part is the workout can be done indoors, outdoors, or on a treadmill.
“Pacing can either be monitored on the treadmill or fitness tracker by speed, which is often displayed as miles per hour (mph) or pace (min: sec per mile),” explains Haines-Landram. “If no technology is available, going off a perceived scale of intensity (how hard the workout feels to you) works.”
Before diving into the workout, we need to clarify some terminology.
- Home Base = If walking outdoors, this is where your area to perform additional exercises that are safe and free from traffic. If walking indoors, this will be next to your treadmill.
- Set = If walking outdoors, one set is either one lap of the distance you set, which should be around 0.25 miles. If walking indoors or on a treadmill, one set will be walking 0.25 miles indoors or on a treadmill.
- Pace = Determine four levels of speed for yourself.
- Level 1 is a slow-paced, casual walk where you can easily hold a conversation and not get winded.
- Level 2 is a faster walk where you can still hold a conversation.
- Level 3 is a fast pace you can sustain for over 10 minutes, but you may not be able to hold a steady conversation because you’re out of breath.
- Level 4 is the fastest pace you can walk before it turns into a run where it’s difficult to talk or hold a conversation.
Haines-Landram says, “The general workout format is to complete one set of roughly 0.25 miles. Then, at your Home Base, complete a lower-body movement and upper-body movement three times, alternating between each.”
Regardless of your fitness level, read on for the workout. Then, check out 5 Best Fitness Tips for Men to Prevent Bone Loss After 60

This is your warm-up, so it’s all about getting the muscles activated and the heart rate slightly elevated. Think of it as setting the stage for the workout to come. A steady five-minute walk at a comfortable pace should do the trick. Then, complete three sets of 10 bodyweight squats and 10 overhead shoulder presses with dumbbells.

It’s time to pick up the pace. At Level 3, you’re going for a brisk walk where you might still be able to chat, but you’d instead focus on your breath. Hold this for about seven minutes. Your heart rate should be higher now, and you’re priming your body for what’s next.
Perform three sets of 10 forward lunges on each leg, alternating with each rep. This can be done by walking or standing in place. Then, do three sets of 10 pushups on the ground, against a wall, or leaning against the treadmill.
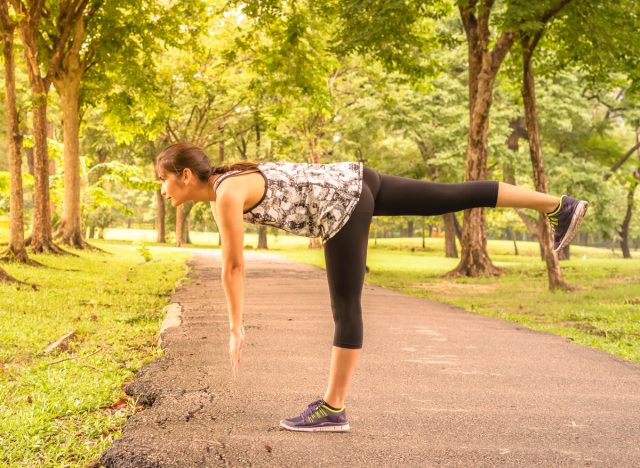
Level 4 is where you push yourself to walk as fast as possible without breaking into a jog. You’ll do this for another seven minutes. Yes, you should be a bit out of breath, and that’s a good thing; it means you’re working hard.
Aim for three sets of five single-leg rear deadlifts (RDLs) on your left leg, then five single-leg RDLs on your right leg. Single-leg RDLs involve balancing on one leg, reaching both hands toward your toes while allowing the other leg to lift off of the ground behind you. The back leg coming off the ground should maintain a straight line with your back, keeping your posterior chain straight. Slowly return to the starting position once you touch your toes (or as close as you can). After that, perform three sets of 10 upright rows with dumbbells.

Let’s dial it back a notch to Level 3 for seven minutes. This is your body’s “reset” period. You’re still moving briskly but allowing your heart rate to recover somewhat. Don’t slack off too much, though. Using a dumbbell, perform one set of 20 thrusters, which involve a squat into a shoulder press in a single explosive movement.

Back to Level 4 we go. Another seven minutes at your quickest walking pace. You’re in the home stretch now, and your body is fully engaged. If you’re not feeling challenged, you need to push harder. At Home Base, do three sets of 10 reverse alternating lunges per leg followed by 10 pushups.

This is the final round of Level 3 for seven minutes. By now, you should be sweating but also basking in the endorphins. It’s your last “reset” period before you cool down, so make it count. Complete three sets of five single-leg RDLs per leg, then 10 upright rows using dumbbells or a kettlebell for an extra challenge.

It’s time for a five-minute Level 2 walk to cool down. You’re back where you started, but your body is anything but the same. You’ve activated muscles, burned calories, and taken a big step—literally—toward sculpting your fittest body. Pat yourself on the back.









