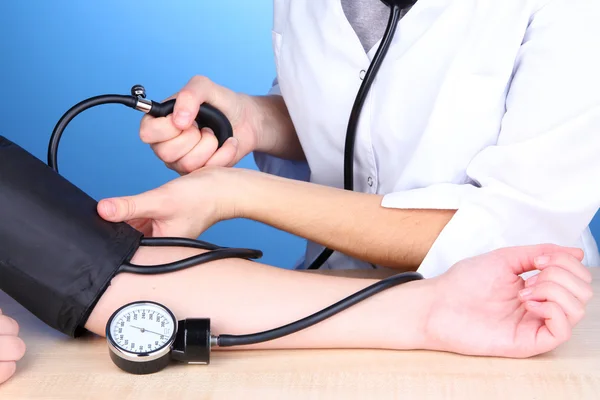
The effects of high blood pressure on cognition are potentially preventable, but the evidence is still evolving.
Here’s what we know:
- High blood pressure is a major risk factor for cognitive decline and dementia. Studies have consistently shown that people with high blood pressure are more likely to experience cognitive problems than those with normal blood pressure.
- Controlling high blood pressure can help to preserve cognitive function. Some studies have shown that controlling high blood pressure can slow down cognitive decline, while others have not shown as strong of an effect. More research is needed to fully understand the impact of blood pressure control on cognitive function.
- The new study suggests a potential new target for preventing cognitive decline in high blood pressure patients. By targeting overactive immune cells in the meninges, it may be possible to prevent the release of IL-17 and protect the brain from damage.
- Other lifestyle changes can also help to protect cognitive function. These include:
- Eating a healthy diet rich in fruits, vegetables, and whole grains
- Exercising regularly
- Getting enough sleep
- Managing stress
Details of the new study
A recent study funded by the National Institutes of Health (NIH) suggests that immune system activity within the brain may play a key role in the cognitive decline associated with chronic high blood pressure (hypertension). This finding, published in Nature Neuroscience, offers promising new avenues for developing treatments that counteract this effect.
The study, led by Dr. Costantino Iadecola and his team, used a mouse model that closely mimics a common form of hypertension in humans. They observed abnormally high levels of interleukin-17 (IL-17), an immune system activator, in the brain and surrounding cerebrospinal fluid. These elevated levels correlated with impaired cognitive function.
Further investigation revealed that IL-17 triggered the activation of brain-resident immune cells called macrophages. Mice lacking the IL-17 receptor on macrophages or depleted of these cells showed no cognitive decline despite having other symptoms of hypertension, highlighting the crucial role of these cells.
Interestingly, the researchers found that the source of IL-17 was not solely the gut, as previously thought. They discovered that immune T cells residing within the dura mater, a protective membrane surrounding the brain, also contributed to IL-17 production. Disruption of the blood-brain barrier in hypertensive mice allowed this IL-17 to enter the brain and activate macrophages.
Blocking the movement of T cells into the meninges or inhibiting their activity restored cognitive function in hypertensive mice, suggesting potential new therapeutic approaches.
Dr. Iadecola emphasizes the two distinct effects of hypertension: “One is IL-17 acting on blood vessels, but this appears to be relatively minor. A more prominent, central effect is caused by cells in the meninges releasing IL-17 that directly affects immune cells in the brain.”
The researchers are now exploring the link between immune cell activation and cognitive decline. They are particularly interested in the potential role of nitric oxide, which was found to be suppressed in both blood vessels and the meninges. Further investigation is needed to determine whether this suppression contributes to tau buildup, a hallmark of Alzheimer’s disease.
The NINDS’s Mind Your Risks® campaign aims to raise awareness about the connection between high blood pressure and brain health, particularly among Black men ages 28-45. This campaign offers strategies for preventing and mitigating the impact of high blood pressure on the brain.
Key Findings:
- Immune system plays a key role: The study found that abnormally high levels of the immune-activating molecule IL-17 in the brain contribute to cognitive decline associated with high blood pressure.
- Two distinct effects: IL-17 acts on both blood vessels and brain macrophages, with the effect on macrophages being more significant.
- T cells in the dura mater are the culprit: These T cells release IL-17, which disrupts the protective barrier around the brain and enters the brain tissue, leading to cognitive impairment.
- Potential new treatment strategy: Blocking the activity of T cells in the meninges restored cognitive function in mice with hypertension, suggesting a new treatment avenue.
Significance:
- This study sheds light on the mechanisms underlying cognitive decline in high blood pressure, offering new avenues for developing therapeutic interventions.
- Targeting T cells in the dura mater could be a promising approach to prevent cognitive decline in people with high blood pressure.
- Further research is needed to confirm these findings in humans and develop effective treatment strategies.
Additional points:
- The study used a mouse model that mimics a common form of hypertension in humans.
- This research builds on previous work showing the link between high salt diet, IL-17, and cognitive decline.
- The NINDS’s Mind Your Risks® campaign highlights the importance of managing high blood pressure for brain health.
Overall, this study offers a significant breakthrough in understanding the link between high blood pressure and cognitive decline, paving the way for potential new therapies to improve brain health.
Continue to check our website soundhealthandlastingwealth.com for more articles of this kind. And, please use our comment section as well, we would love to hear from you.