DR ELLIE CANNON: Last week I announced on national television that I take antidepressants. I was talking to Phillip Schofield and Holly Willoughby on This Morning during my regular slot answering health questions, and the subject came up.
I noted that, while many millions of people in Britain rely on antidepressants, there’s a certain stigma that surrounds them. Given that they help people cope with sometimes crushing mental health symptoms, and live their lives to their fullest, it’s ridiculous that anyone should feel ashamed in any way, in my view.
So I felt it only right to admit that I, too, take them – as I used to suffer very bad anxiety. It means I don’t know.
There are many ways to deal with mental illness, including therapy and lifestyle changes. But for many, including me, medication is a valid and effective answer, and people shouldn’t be afraid to try it.

Dr Ellie Cannon appeared on This Morning during the week to tell Holly and Phil about her experiences taking anti-depressants and why there is no shame in seeking help
My lawyer son claims marijuana calms him. But is he an addict?
My 34-year-old son is an intelligent, hard-working lawyer and a lovely, charming man.
But in the past year he’s started smoking a lot of marijuana. He says it’s to relax, but I don’t think he seems like himself.
Could he be addicted?
Marijuana , or cannabis, is in common use in the UK despite it being an illegal drug. Many people say they use it to help reduce stress and pain as well as for relaxation. But cannabis use is not risk-free. We do know, and I have witnessed as a GP, that cannabis can also make people unwell, paranoid, confused and anxious.
It is an addictive drug if someone is using it regularly, and can lead to withdrawal symptoms when stopped. These include nausea, irritability, insomnia and sweating.
Cannabis is associated with an increased risk of psychosis-like illnesses such as schizophrenia, where people believe things that are not true, or see things that are not there. This is more likely in someone using it for a long time from a young age. It can also have effects on breathing, can worsen asthma and is known to reduce sperm count.

A reader has written to Dr Ellie to ask whether her solicitor son is addicted to cannabis after he admitted smoking the drug regularly to relax
If someone has started using a drug more frequently and undergone mood changes it is natural to assume that the changes are related to the drug use. However, as a doctor I would question why they are starting to use the drugs more often. If someone is self-medicating to relieve pain or stress, it might be these things, rather than the drug, that’s causing mood changes.
As relatives and carers we are in a unique position to ask these questions in a non-judgmental way, and give our loved ones the chance to open up and get the support they need. New drug use, particularly in a young man, can be the sign of background mental health issues such as depression and anxiety. Frank is the national service for all drug users and information, and can be contacted 24/7 on 0300 1236600.
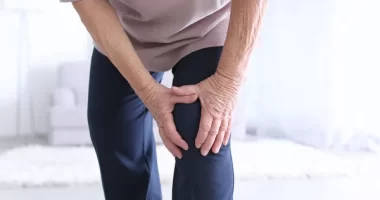
I am a 74-year-old man who exercises for two hours a day, six days a week.
My knees and shoulders have started to hurt more recently, and I was wondering if you could advise me on any supplements I should be taking.
I already take omega-3 capsules, but I’ve heard turmeric helps this sort of discomfort.
Vitamin pills are hugely popular, and some people spend a small fortune on them every month.
More from Dr Ellie Cannon for The Mail on Sunday…
But that doesn’t mean there is scientific evidence to prove they work. It’s for this reason that, generally speaking, doctors don’t recommend them.
Joint supplements tend to work in some people and not others and that’s why we no longer prescribe any on the NHS.
If a patient tells me they want to try a supplement, I suggest they take the same brand and same dose for two to three months. If they feel the benefit, then it’s worth continuing.
Studies into omega-3 fish oil supplements suggest they improve the symptoms of rheumatoid arthritis, but not particularly osteoarthritis, the most likely cause of knee and shoulder pain in older people.
However, fish oil and omega-3 is a rich source of Vitamin D which we know is important for maintaining healthy joints and bones.
Turmeric is believed by many cultures to have anti-inflammatory properties, although again there is very limited scientific evidence to suggest its benefits. It is likely to have minimal side effects, but could increases the effects of blood-thinners. Small trials have shown that turmeric may improve pain and knee function.
If someone wants to try it, I would suggest discussing it with a pharmacist first.
Every couple of years, I have my ears vacuumed at the hospital. The last time I went, about a month ago, I was told that it was the final time they’d be offering the treatment.
What am I going to do instead?
Ear wax treatments have changed over the past few years, which has upset many people as ear wax build-up can cause hearing loss, earache and even tinnitus or vertigo.
Some people are more prone than others, and it’s particularly a risk in those who use hearing aids. A few years ago the old-fashioned syringing – a large metal syringe was used to shoot a jet of water into the ear, which dislodged the wax – was stopped. This was due to potential damage to ear drums.
The treatments we safely use now involve either irrigation, which is basically the same as syringing, but uses a machine to project a controlled amount of water into the ear, or vacuum suction, known as microsuction, where it is sucked out.
A reader has been told that they will no longer be offered treatment to remove earwax in future
Many GP practices ceased doing these things over the past few years as local NHS funding for it was stopped. Around the country this has been a controversial decision. Many patients rely on this treatment, which may seem trivial but really isn’t.
Certain high street shops do offer microsuction safely, at a reasonable price.
Other options to remove wax, which a pharmacist can offer advice on, are to use olive oil or sodium bicarbonate drops that soften or break down the wax to help it pass out naturally.
£250million won’t fix our GP crisis
Health Secretary Sajid Javid revealed his new blueprint to address the GP crisis and get doctors seeing patients face-to-face again – including injecting £250 million into practices to recruit more GPs.
Financial support – it works out at £30,000 per surgery – is welcome. But it won’t be a quick fix. Patients need us more than ever, with annual GP appointments rising by ten per cent since 2019.
More people are suffering with chronic diseases such as diabetes, but we’re also increasingly relied upon for logistical things such as travel insurance letters.
I’m not making excuses for surgeries that shut up shop: I’ve been a victim of this, as a patient, myself. But we must avoid GPs being stretched too thinly.
Patients can play their part by seeing a pharmacist or nurse where appropriate, leaving doctors with time to see those who really require our help.
You May Also Like
Post source: Daily mail