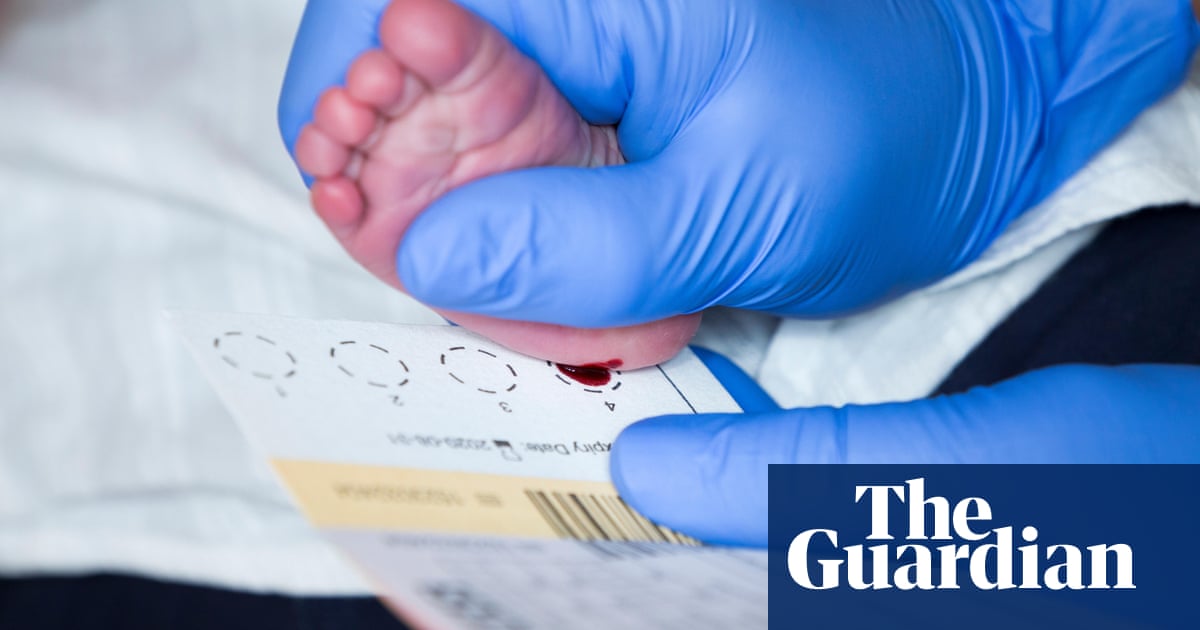
The word “breathe” has never been more potent than at the moment.
The instruction to breathe is something midwives say an awful lot to women in labour. It’s also being said a great deal to patients on ventilators whose lungs have been taken over by Covid-19.
In the hospital where I work as a midwife, there are double doors leading from our midwifery unit to a makeshift intensive care unit. On one side, I am involved with the unborn who are yet to breathe, while on the other there are people unable to breathe independently. The proximity of brand new life and end of life separated by double doors is very affecting for me and all my colleagues.
The women I look after must be aware, but when they are allocated a delivery room, they are completely absorbed in giving birth. It’s almost a holiday from the shitstorm. These are strange times we are working in, but I haven’t felt frightened, and neither should the women I’m helping.
Antenatal classes are online and a lot of care is delivered by telephone; it seems to have worked very well. If a woman has to come in, our emergency obstetric unit is open, but anybody else attending must wait outside. Most birth partners have been incredibly understanding, given that we don’t even provide chairs in the corridor outside. Often, there’s a line of physically distanced people.
More women have started asking to have an induction or elective caesarean section to try and gain a bit of control in the circumstances. Once someone is in established labour, the birth partner can stay until delivery. We try and keep people in there as long as possible, but it depends how many people are in at one time. Once the woman leaves and goes into postnatal care, it’s goodbye to the birth partner at the doors. The only exceptions we’ve made have been when the woman is experiencing mental health issues.
More people have been delivering babies in the car park than usual. It’s always been the third most popular place after the delivery suite and antenatal wards. People are leaving it to the last minute because of fears around coronavirus. More are coming in in advanced labour; some decide to stay at home until they get anxious and come into hospital.
The postnatal ward is a lovely place to be at the moment. The curtains are open, and women are helping each other and bonding in a way that we thought was a thing of the past. One of the things we will probably review is how often partners are allowed in. Now that is not happening, there is a spirit of female empowerment and togetherness. Those who have had babies before are helping first-timers with breastfeeding, for example. There is also the ability to share stories and to come to terms with your birth experience.
There have been cases of stillborn babies and the key thing that has changed is the way in which the death is registered. There’s a lot more having to be done online. Once a child has been separated from the mother there is no further opportunity to see the baby.
It is difficult, but not necessarily in the most obvious way. Sometimes, at the point of delivery women don’t want to see their stillborn baby; they’re completely and utterly closed to the idea and then change their mind a day later. Managing that situation requires sensitivity. We have very good bereavement midwives who are experienced in helping women down this road.
We’ve been 20% down on the workforce generally, and have had to call in agency staff. It’s a busy unit anyway but it has felt most of the time like we’re slightly ahead of it going completely pear-shaped. We’re nine weeks into this crisis. It’s amazing what you get used to.
We are wearing various degrees of personal protective equipment (PPE). For women with coronavirus, we wear full PPE. It’s very hot. It’s also alienating because a huge amount of our job, which has a massive bearing on the woman’s experience, is done through eye contact, voice, movement and being able to read people’s facial expressions.
Panic has a huge impact on a woman’s perception of her experience. If you’re looked after by someone in a visor, where all you can see is a reflection of the window, you’re not seeing physical cues. The lack of human touch is another unfortunate consequence of PPE.
I became a midwife 10 years ago when I was in my mid-50s for political reasons, namely to support the NHS. Sadly, the biggest social change I have lived through has been the gradual denigration of the health service. I’ve benefited my entire life from an excellent welfare system. My father died very young having had fantastic treatment, and my husband died of cancer aged 44. He also received brilliant care which didn’t cost one penny.
As a midwife, every transaction I have with a woman and her family is a political one. I am the NHS when someone gives birth. By providing the service that I do, I feel I am making a persistent political statement that we should safeguard the amazing gift of our health service.
Angela Barry is a midwife in a London hospital
The Guardian